The knee is a large and complex joint. It connects the femur to the tibia. It also has other surrounding structures like the tibia and kneecap.
The knee plays a very important role in various bodily functions and movements such as walking, running, and jumping. The complexity of the structure of the knee makes it susceptible to pain. The middle part of the knee experiences most of the pain.
Medial knee pain occurs for a variety of reasons. The common medial knee pain causes include the following:
MCL Tear (Medial Collateral Ligament)
some or all of the fibers of the MCL on the inner side of the knee are damaged. The patient complains of a sudden yet severe medial knee pain. There is also bruising, swelling, stiffness, and instability. The pain is worsened when walking, climbing the stairs, or bending the legs. (1, 2)
Meniscus Tear
It is also known as the medial cartilage tear. It is characterized by a tear in the cartilage lining of the inner side of the meniscus (knee joint). The pain is sudden. The patient finds it difficult to straighten the legs. There is also swelling and instability. Simple activities can trigger medial knee pain such as walking, climbing the stairs, squatting, and running. (3)
Pes Anserine Bursitis
It is the less common cause of medial knee pain. It is characterized by inflammation of the pes anserine burse, a small fluid-filled sac. If there is an inflammation, the fluid that reduces friction in the knee bones gets dry leading to pain and inflammation, especially when moving.
The onset of the pain is sudden and gradually intensifies. The pain is more intense when the patient tries to climb the stairs. It commonly affects overweight middle-aged women as well as swimmers and runners.
Arthritis
It is a medical condition characterized by wear and tear of the cartilage that lines the medial side of the joints. The one that causes medial knee pain is osteoarthritis. Medial knee pain worsens as the person grows old.
Patients 50 years old and above are prone to osteoarthritis. The clinical manifestations include inside knee pain, a stiffness of the joints in the early morning, reduced movements of the legs, and swelling. The patient also complains of chronic medial knee pain. The patient is aggravated by cold weather and prolonged activity or rest. The severity of symptoms depends on whether osteoarthritis is mild, moderate, or severe. (4, 5)
Medial cartilage meniscus injury
A torn meniscus causes pain on the inside structure of the knee. This type of injury is common in athletes, especially in contact sports such as basketball.
Knee contusion
It occurs because of a sudden impact on the side of the knee. In layman’s term, it is called bruising of the knee. It may sound simple on the outside but it could cause damage to the soft tissues and even to the bones. (2)
Medial knee pain is common because the muscles in the knee area are extremely sensitive. If the muscles become weak or tight, it affects the way the knee moves. More force will go through the inner side of the joints leading to damage to the inner side of the knee.
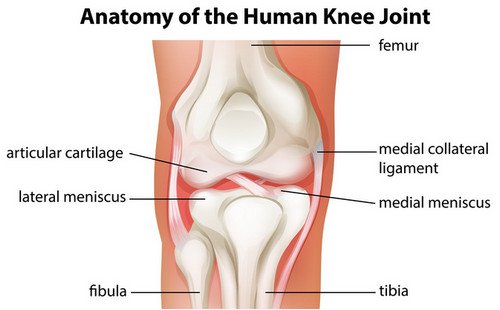 Image 1: Anatomy of the knee joints.
Image 1: Anatomy of the knee joints.
Photo Source: progressivephysio.com

Picture 2: MCL tear which is one of the cause of medial knee pain.
Image Source: www.knee-pain-explained.com
Photo 3: A knee brace, supports the knee, keeps the knee in placed, and prevent further injury to the knees.
Picture Source: www.physioroom.com
Medial knee pain treatment
Inflammation is the body’s way to cope with injury. When it comes to treating medial knee pain and knee pain in general, one of the primary goals is to break the inflammatory response. If the inflammation is not resolved the soonest time possible, it could lead to chronic medial knee pain and severe injury to the knee.
It makes the treatment quite difficult considering that the infection has already advanced. The goal of the medial knee pain treatment is to control the substance that causes inflammation and limiting movements that could further injure the knee. (3, 4, 5, 6)
The first treatment approach for knee pain is protection, rest, ice, compression, and elevation (PRICE).
- Protection – It is important to protect the knee from further trauma. To protect the knee, a split or knee pad should be used. A pad over the knee can help control the symptoms of knee injuries.
- Rest – Do not move the injured knee to significantly reduce the strain and give ample time for the injured knee to heal.
- Ice – Cold compress helps reduce swelling and inflammation.
- Compression – A medial knee pain brace reduces swelling, keep the alignment of the patella, and keep the joint mechanic intact.
- Elevate – By simply elevating the knee, swelling can be reduced and blood circulation will be improved significantly. (4, 6, 7)
Pain Management
Over the counter pain medications are used to control the pain. If the pain does not go away, then the doctor will prescribe stronger pain medication.
Pain medications do not only control the pain but also help alleviate inflammation and facilitate in the breaking of an inflammatory cycle. If you have stomach ulcers or bleeding problems, you should not use non-steroidal anti-inflammatory drugs.
Medial knee pain exercises
There are various exercises for medial knee pain. However, exercises should only be done if the injury is not painful to touch and not painful to stretch. If there is an intense pain even when the patient is at rest, then the patient should refrain from doing any types of exercise.
Before starting any forms of exercise for the knee pain, you have to make sure you consult your doctor. If you exercise without consulting your doctor, you could be adding injury to the knees. (7, 8, 9, 10)
When should you call out for professional help?
If you have tried all the treatment remedies mentioned above but still the pain does not go away, then it is high time to consult your doctor. The doctor or physical therapist will further evaluate the pain.
The more you need to talk to your doctor if the knee pain gets intense, you have a fever, and you are feeling sick. If there are signs of infection, then you need to go to the emergency room to immediately treat the underlying condition and prevent secondary infection. (2, 6, 10)
References:
- http://www.sportsinjuryclinic.net/sport-injuries/knee-pain/medial-knee-pain
- https://www.healthline.com/health/inner-knee-pain
- http://www.knee-pain-explained.com/medial-knee-pain.html
- http://www.londonorthopaedic.com/medial-knee-pain/
- https://www.injurytreatment.com.au/injury-information/knee/medial-inside-knee-pain/
- https://www.braceability.com/blog/types-of-knee-pain-anterior-posterior-medial-lateral-knee-pain/
- https://www.webmd.com/pain-management/guide/knee-pain-overview#1
- https://www.thekneepainguru.com/inner-knee-pain/
- https://en.wikipedia.org/wiki/Medial_knee_injuries
- http://mobilitymastery.com/how-to-relieve-medial-knee-pain-low-back-si-pain-groin-pain-more
