Neuritis Definition
Neuritis is a medical term for inflammation of the nerve. It can affect one nerve (mononeuritis) or more nerves (plexitis).
A mononeuritis multiplex is when several single nerves are affected. On the other hand, a polyneuritis is when separate nerves are affected. (2)
Neuritis Symptoms
- Tingling sensation
- Pain (burning, pricking, or stabbing sensation) is worst at night and aggravated by touch and change in temperature
- Muscle weakness (paresis) (2)
- Noticeable changed in the muscle tone
- Tenderness
- Muscle atrophy (muscle wasting) (3)
- Abnormal sensation (paresthesia)
- In severe case, loss of sensation and paralysis

Image 1: An Image showing how a peripheral neuritis looks like
Picture Source: www.peripheralneuropathytreatments.com
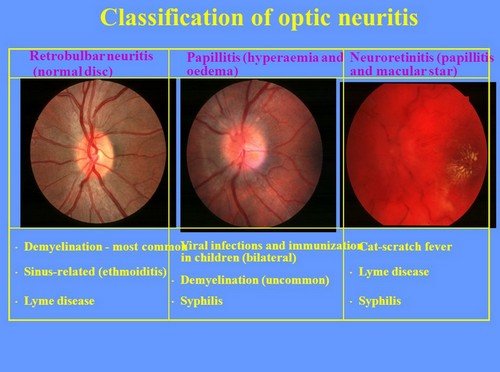 Photo 2: The different classifications of optic neuritis
Photo 2: The different classifications of optic neuritis
Picture Source: slideplayer.com

Image 3: A clinical presentation of a patient suffering from ulnar neuritis
Photo Source: www.coen1.org
What are the causes of neuritis?
- Injury – An injury to the nerve causes neuritis. It could be a physical injury, chemical injury, or radiation injury. An example of physical injury to the nerve is carpal tunnel syndrome or pain and numbness of the thumb and index fingers. On the other hand, chemical nerve injury arise secondary to damage to the surrounding structures causing the nerves to release noxious substances. Radiation injury develops after radiotherapy. (1)
- Nutritional Deficiencies – Neuritis is common in people with vitamin B complex deficiency, specifically vitamin B1, B2, B6, and B12.
- Infections – Some diseases causes inflammation to the nerves such as syphilis, leprosy, chicken pox, Lyme disease, diphtheria, cat scratch disease, and herpes simplex infection.
- Predisposing factors – Some medical conditions increase your chance of experiencing neuritis. Examples are hypothyroidism, diabetes mellitus, pernicious anemia, porphyria, chronic acidosis, certain types of cancer, and autoimmune disease like multiple sclerosis and systemic lupus erythematosis. (4, 5)
- Genetics – Some types of neuritis can be transferred genetically such as amyloid neuropathy and Leber’s hereditary optic neuropathy.
- Toxins and medications – Neuritis can be triggered by toxicity such as exposure to heavy metals, environmental pollutants, strong chemicals, drugs, chronic alcoholism, and lead. Some antibiotics cause neuritis. (3, 5)
Types of Neuritis
Optic neuritis
It is an inflammation of the optic nerve. Optic nerves are nerve fibers responsible for transmitting visual information from the eyes to the brain. The most common optic neuritis symptoms are pain, visual field loss, loss of color vision, seeing flashing lights, and temporary vision loss in one eye.
It is usually associated with multiple sclerosis, lupus, and other types of immune disease. Neuritis treatment for optic neuritis includes steroid medications to hasten the healing process. To accurately diagnose the condition of the patient, the doctor will conduct a thorough examination as well as checking the past medical and past surgical history of the patient.
The eyes will be thoroughly checked by the ophthalmologist. If the doctor is suspecting multiple sclerosis, a magnetic resonance imaging (MRI) procedure is ordered. This is to check for the presence of lesion, which will confirm multiple sclerosis. Blood works will be done too. (3, 10)
Peripheral neuritis
It is the inflammation of the peripheral nerves. Symptoms include pain, numbness, and weakness in the hands and feet. It may also affect other parts of the body. The pain is stabbing and tingling in nature. The doctor will usually prescribe pain reliever to reduce the pain. (6)
Brachial neuritis
It is the inflammation of the brachial plexus. The patient complains of sudden onset of pain in the shoulder and arm followed by numbness and weakness. The pain is sudden and severe in nature. The pain starts from the shoulder and radiates to the upper arm.
Patient describes the pain as sharp, feels like there’s a piercing on it, and radiates to the adjacent parts of the body. The symptoms are felt in one side of the body. The intense pain goes on for a few days. Then, the arms become weak.
There is a noticeable wasting of the muscles, but eventually gets better with time. If not addressed accordingly, the condition will worsen leading to partial or complete paralysis of the arm. (7, 8)
Intercostal neuritis
The pain is felt along the intercostal nerves, in between the ribs. The cardinal signs and symptoms are dull and constant pain. Some patients experienced sharp and stabbing pain. The pain is felt during sudden movements, especially actions that involve the upper chest. Simple breathing, laughing, and sneezing can trigger the pain.
Associated symptoms include left-sided pain, tingling sensation, numbness, and shooting pain that radiates to the back. Severe cases of intercostal neuritis caused extreme pain, which makes it difficult for the patient to breathe and move.
If you are feeling pain in the intercostal area as well as its surrounding structure, you should immediately call for help.
Lumbosacral neuritis
It pertains to the inflammation of the lumbar nerves. There are several nerves in the lumbar area. It carries both sensory and motor impulses if you are experiencing lumbosacral neuritis, it means that there is something wrong in the lumbar nerve fibers.
Ulnar neuritis
It is also called cubital tunnel syndrome. It pertains to the inflammation of the ulnar nerve. It causes numbness and muscle weakness in the hand. (8)
Vestibular neuritis
It is a sudden pain and dysfunction of the peripheral vestibular system. Other symptoms include nausea with vomiting, and vertigo. Labyrinthitis neuritis and vestibular neuritis are somehow related, but the latter is distinguished because of its preserved auditory functions. Vestibular neuritis is actually not inflammatory in nature. Hence, most health care professionals call it vestibular neuropathy.
Vestibular neuritis treatment includes medication to hasten the healing process, hydration to prevent dehydration, and bed rest. To avoid further episodes of vestibular neuritis, the patient is highly discouraged to drink alcoholic beverages, avoid bright lights, cut out the noise, and anything that causes stress. (4)
Occipital neuritis
It is typically a form of headache causing pain in the upper neck and at the back of the head. The pain targets the occipital nerves. It is aching, throbbing, and burning in nature.
The patient feels like a sharp object stabs in the occipital area of the head. It is usually associated with inflammatory changes affecting the occipital nerves. (6, 7, 8, 9)
Other least common types of neuritis are cranial neuritis, arsenic neuritis, and granulomatous neuritis of leprosy.
References:
- www.mayoclinic.org
- https://en.wikipedia.org
- www.healthhype.com
- www.healthline.com
- www.medicinenet.com
- https://my.clevelandclinic.org
- www.webmd.com
- www.allaboutvision.com
- www.diagnose-me.com
- Neuritis: New Insights for the Healthcare Professional: 2013 Edition Scholarly Paper



